Intumescent Cataract: Understanding the Swollen Lens and Your Vision
บทความโดย: seoteam seoteam วันที่อัพเดท: 15 May 2569

An intumescent cataract is not just your typical cloudy lens. It represents an advanced stage of a cataract where the lens becomes significantly swollen with fluid. If left untreated, it can lead to severe pressure within the eye and permanent vision loss. Understanding this condition is the first step toward reclaiming clear sight.
Key Takeaway
- An intumescent cataract occurs when the eye's lens absorbs excess fluid and swells, often leading to increased ocular pressure.
- Common symptoms include rapid vision decline, severe eye pain, and visible milky-white discoloration of the pupil.
- Timely cataract surgery is the only effective treatment to prevent secondary conditions like glaucoma.
- Modern surgical techniques like phacoemulsification and high-quality IOLs make recovery faster and safer than ever.
Table of Contents
An intumescent cataract is a specific type of mature cataract characterized by the hydration of lens fibers. As the lens proteins break down, they draw in water via osmosis, causing the lens to expand in size. This swelling can narrow the space in the front of the eye, potentially triggering angle-closure glaucoma, a medical emergency. Unlike a standard cortical cataract, which involves localized opacities, an intumescent cataract involves the entire lens structure.
Because the lens is physically changing shape and size, the symptoms are often more dramatic than early-stage cataracts:
- Rapid Vision Loss: A noticeable and quick decline in the clarity of your vision.
- Severe Eye Pain: Often caused by increased pressure within the eye.
- Headaches and Nausea: Frequently associated with the onset of secondary glaucoma.
- Visible White Pupil: The eye may appear to have a milky or pearly-white "marble" in the center.
- Halos and Glare: Extreme sensitivity to light, especially at night.
The primary cause is the natural progression of an untreated cataract. However, specific factors can accelerate this swelling:
- Advanced Age: The most common factor as lens proteins naturally degenerate over time.
- Trauma: Physical injury to the eye can rupture the lens capsule, leading to rapid fluid absorption.
- Diabetes: High blood sugar levels can alter the osmotic balance in the eye, causing the lens to swell.
- Long-term Steroid Use: Certain medications are known to speed up cataract maturation.
While not all cataracts can be prevented, especially those linked to aging or genetics, there is a great deal you can do to reduce your risk and slow their progression.
- Wear UV-protective eyewear whenever you're outdoors. Sunglasses with 100% UVA and UVB protection are one of the simplest and most effective tools for long-term eye health.
- Use appropriate protective eyewear at work if your environment involves heat, infrared radiation, or electrical hazards. Industrial eye shields and specialized goggles can significantly reduce occupational exposure risk.
- Manage systemic health conditions diligently. Keeping blood sugar under control if you have diabetes, for instance, goes a long way in protecting the health of your eye's lens.
- Limit alcohol consumption and avoid smoking, both of which are associated with higher rates of cataract formation. Oxidative stress caused by these habits damages the proteins in the lens over time.
- Maintain a nutrient-rich diet with antioxidants such as vitamins C and E, lutein, and zeaxanthin. These nutrients help protect the lens from oxidative damage and are found in leafy greens, citrus fruits, and eggs.
- Schedule regular eye examinations, even if you currently have no symptoms. Early detection allows for monitoring and timely intervention before the condition becomes advanced.
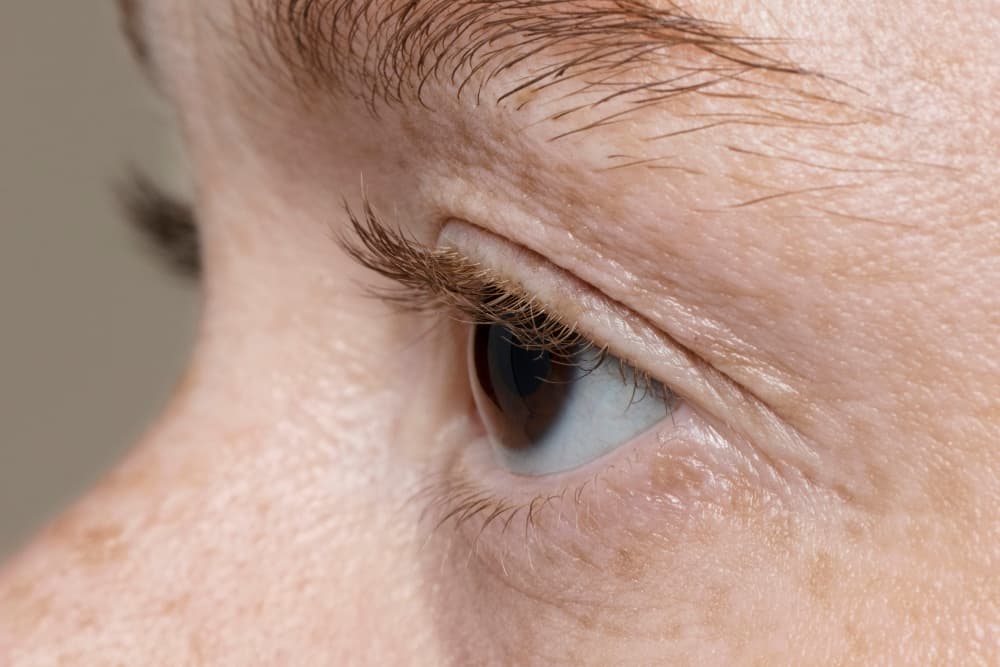
Diagnosing an intumescent cataract requires a comprehensive evaluation by an eye care professional. The examination typically involves several steps.
- Slit-lamp biomicroscopy is the cornerstone of cataract diagnosis. This specialized microscope allows the ophthalmologist to examine the lens in detail, assessing its degree of opacification, swelling, and position.
- Visual acuity testing measures how clearly you can see at various distances, helping quantify the extent to which the cataract is affecting your functional vision.
- Intraocular pressure (IOP) measurement is critical when an intumescent cataract is suspected, as elevated pressure may indicate the onset of secondary glaucoma.
- Anterior segment imaging can help visualize the dimensions of the swollen lens and assess how much it is encroaching on the anterior chamber of the eye.
- Ultrasound B-scan or biometry may be used when the degree of lens opacity makes direct visualization difficult, and also helps in planning surgical treatment by calculating the correct IOL power for implantation.
- Gonioscopy, a technique used to assess the drainage angle of the eye, may be performed if angle-closure glaucoma is a concern.
The only way to treat an intumescent cataract is through cataract surgery. Because the lens is swollen and under pressure, these cases require an experienced surgeon.
- Phacoemulsification: This is the gold standard. The surgeon uses ultrasonic energy to break up the swollen lens and remove it through a tiny incision.
- IOLs (Intraocular Lenses): Once the natural lens is removed, it is replaced with an artificial lens. Modern IOLs can correct nearsightedness, farsightedness, and even astigmatism, often resulting in better vision than before the cataract developed.
An intumescent cataract is a serious condition, but it is highly treatable. By choosing a timely cataract surgery, you not only restore your vision but also protect your eye from the risks of high pressure and glaucoma. If you notice your vision blurring or a white clouding in your eye, consult an eye specialist immediately to discuss phacoemulsification and your options for IOLs.
What are the common symptoms associated with intumescent cataracts?
The most common symptoms include a sudden drop in vision, a milky-white appearance in the pupil, and eye pain or headaches caused by increased intraocular pressure. You may also experience significant glare and halos around lights.
Are there specific risk factors linked to the development of intumescent cataracts?
Yes. Significant risk factors include advanced age, poorly managed diabetes, previous eye trauma, and neglecting regular eye check-ups, which allows a standard cataract to progress to the advanced intumescent stage.



